My wife was hospitalized recently and, while spending time with her, I couldn’t help but notice how much time the nurses and doctors spent looking at their computer screens.
I know hospital leaders are looking for ways to reduce the time clinicians spend on technology-related tasks, but seeing nurses absorbed in computer work when I was trying to get one of them to attend to my wife’s care is an entirely different matter.

A week or so later I noticed an article headlined, “Report: EHRs receive more face time with physicians than patients do.” The article summarized the results of a study published in Health Affairs that found that physicians spent an average of more than three hours daily on office visits and slightly more time on what was described as “desktop medicine,” which includes tasks such as typing notes into the electronic health record (EHR).
I would say that nurses spend more time on computers than with patients, too, based on observing the nurses during my wife’s hospital stay and in discussing nursing care with hospital leaders across the nation. Our perception is supported by a University of Pittsburgh Medical Center study that found nurses spending about a third of their time interacting with technology versus only 16 percent on patient interaction and care.
I’d be the first person to attest to the value of the information clinicians obtain from EHRs. But EHRs and other kinds of health care technologies were supposed to free up time for providers, remember?
New technological breakthroughs help caregivers work more efficiently – and effectively
Technology will never replace caregivers; the need and desire for humans to observe, heal, advise and console is too great. But technology can certainly assist. And it can help in ways that can make care providers more efficient – and, more importantly, in ways that make them more effective in providing care.
As the Vitalacy team helps hospitals implement our patient safety platform and technology, we have seen up close the challenges our clients face in gaining buy-in and support from clinicians. Deploying new technology is a difficult challenge that centers on understanding human behavior and the interface between humans and technology in health care settings. Finding the proper balance between technology and humanity is a delicate act.
Sometimes, there is a mistaken belief at first that our technology is an “overwatch” system – that is, one that monitors the workflow of caregivers to find fault. Rather, our system is designed to assist clinicians to increase the effectiveness of the care they provide by observing and trending their movements from location to location during their shifts – where they are working and for how long.
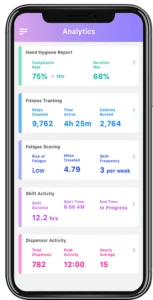
Once these real-time data are summarized into easy-to-understand graphics and reports, they provide care providers and their managers with insights that help them prevent healthcare-acquired infections and conditions, such as falls with harm, pressure ulcers, and venous thromboembolism (VTE) (Vitalacy, July 9, 2019).
For example, insights gained from the data provided by our patient safety platform helped an academic medical center to improve hand hygiene compliance, which in turn reduced healthcare-acquired infections for two consecutive quarters (Vitalacy, Mar. 14, 2019). These data also can help hospitals to identify caregivers who have been on their feet for too long and show signs of nurse fatigue, giving them welcome relief, improving their well-being, and reducing the chances of a medical error.
Improving patient safety is a two-way street
The interface between technology and care providers makes both work more effectively, as does the interface between Vitalacy and our clients. Working collaboratively with our clients is foundational to the success of our patient safety platform. With each of our clients, we establish a work group to assure essential bi-directional communication between us.
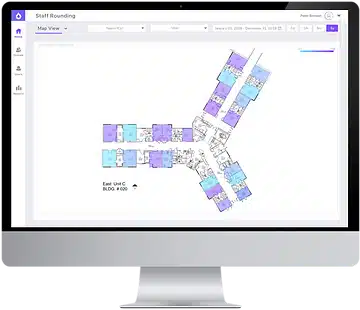
This kind of collaboration led to the development of our purposeful rounding data module, which tracks when and for how long caregivers interact with patients. One of our client’s nursing leaders suggested using our hand hygiene compliance tracking to track when and for how long care providers interacted with patients (Vitalacy, Mar. 14, 2019). Now, by viewing activity by staff and room, managers using our platform can ensure that care providers get alerts when patients have not been visited as necessary; this information also helps managers to identify high- and low-performing staff to target education and training.
Vitalacy’s core competency is the ability to track workflow to gather information that helps our clients provide patient care more effectively. We’re in the business of effectiveness – creating the data to assure an effective and highly reliable work environment – one in which both patients and family members can feel safe and confident.
Once hospital leaders and care providers understand that our platform gives them a collaborative opportunity to create that high reliability environment, they’ll all in.
Request a demo of Vitalacy’s Automated Hand Hygiene Monitoring Solution today!
References
Higgens, L, et al. Hospital nurses’ activity in a technology-rich environment. Journal of Nursing Care Quality, July/Sept. 2017, 32(3):208-217.
Nour-Omid, J. What do VTE, pressure ulcers, falls and adverse drug events have in common? Vitalacy blog, July 9, 2019.
Rupp, S. Report: EHRs receive more face-time with physicians than patients. NueMD Industry News, April 18, 2017.
Tai-Seale, M, et al. Electronic medical record logs indicate that physicians split time evenly between seeing patients and desktop medicine. Health Affairs, April 2017, 36(4).
Vitalacy, Inc. Finding new ways to prevent healthcare-acquired infections and conditions. Mar. 14, 2019.
Author
-

Vitalacy is committed to reducing patient harm in healthcare through better hand hygiene and patient safety solutions. Bluetooth-enabled smart sensors and wearables help improve outcomes and Leapfrog Hospital Safety Grades.
View all posts




